Dosage calculation formula is one of the most important concepts in pharmacy, nursing, and clinical practice. Accurate dosage calculations are essential to ensure that patients receive the correct amount of medication. Even a small mistake in dosage calculation can lead to serious health complications, including overdose or underdose.
In healthcare settings, professionals deal with different types of medications, strengths, and dosage forms. Therefore, understanding the dosage calculation formula is critical for safe and effective patient care. Students often find this topic challenging due to unit conversions, formula confusion, and lack of practice.
This complete 2026 guide will help you understand dosage calculation formula in a simple and practical way. You will learn formulas, step-by-step examples, methods, and tips to avoid common mistakes.
What is Dosage Calculation?
Dosage calculation refers to the process of determining the correct amount of medication to be administered to a patient based on factors such as age, weight, condition, and drug strength.
The dosage calculation formula helps convert prescribed doses into measurable quantities like tablets, milliliters, or injections.
Basic Dosage Calculation Formula
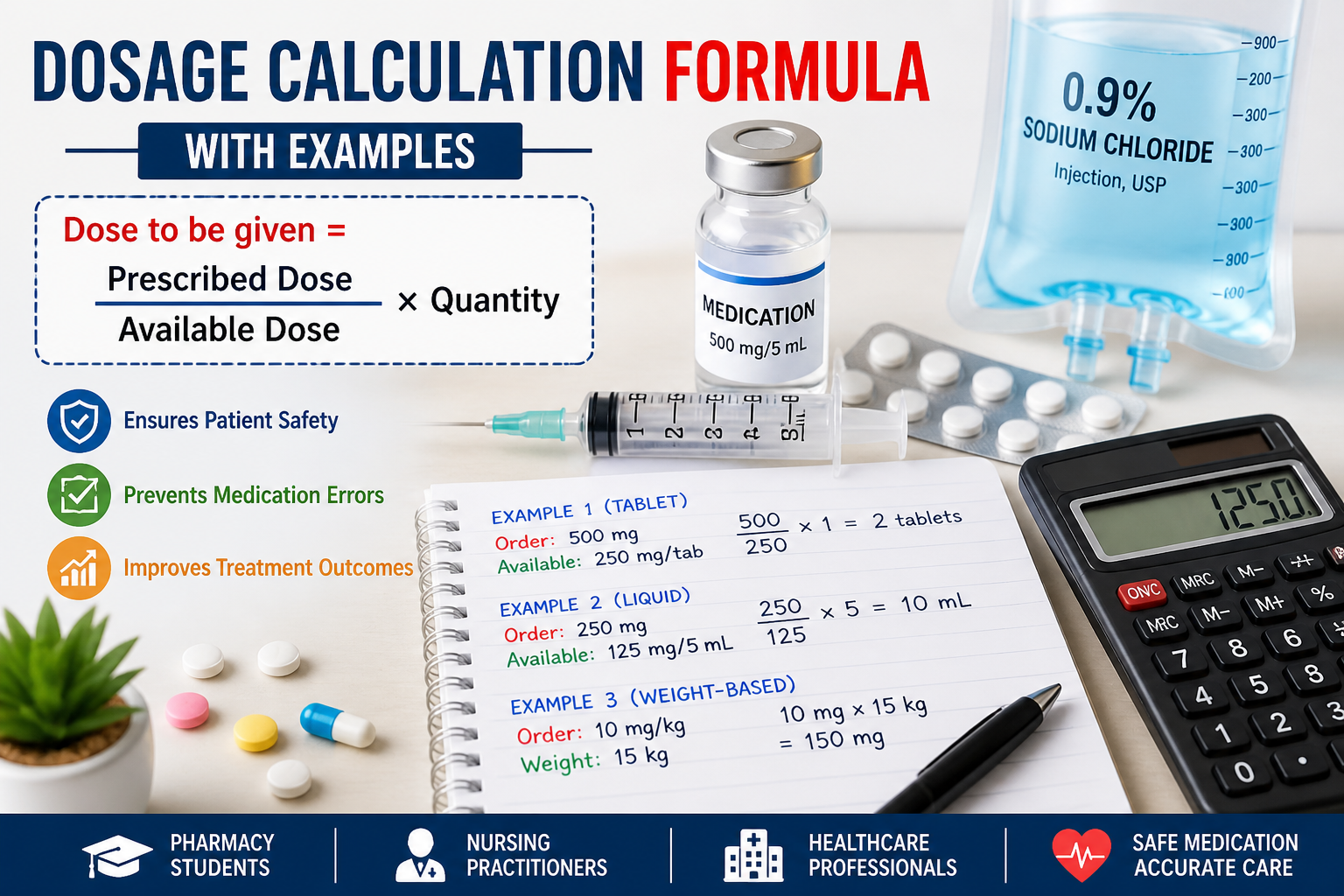
The most commonly used dosage calculation formula is:
Dose to be given=Prescribed DoseAvailable Dose×Quantity\text{Dose to be given} = \frac{\text{Prescribed Dose}}{\text{Available Dose}} \times \text{Quantity}
Explanation:
- Prescribed Dose = Doctor’s order
- Available Dose = Strength of drug available
- Quantity = Form (tablet, mL, etc.)
Types of Dosage Calculation Formula
1. Tablet Dosage Calculation
Used when medication is available in tablet form.
Example:
Doctor orders 500 mg
Available tablet = 250 mg
Solution:
(500 ÷ 250) × 1 = 2 tablets
2. Liquid Dosage Calculation
Used for syrups or injections.
Example:
Order = 250 mg
Available = 125 mg per 5 mL
Solution:
(250 ÷ 125) × 5 = 10 mL
3. Injection Dosage Calculation
Used for IV or IM injections.
Example:
Order = 1 g
Available = 500 mg
Solution:
(1000 ÷ 500) = 2 doses
Weight-Based Dosage Calculation Formula
Weight-based dosing is common in pediatric and critical care.
Dose=Weight (kg)×Dose per kg\text{Dose} = \text{Weight (kg)} \times \text{Dose per kg}
Example:
Child weight = 10 kg
Dose = 5 mg/kg
Solution:
10 × 5 = 50 mg
Body Surface Area (BSA) Dosage Formula
Used in chemotherapy and special treatments.
BSA=Height (cm)×Weight (kg)3600\text{BSA} = \sqrt{\frac{\text{Height (cm)} \times \text{Weight (kg)}}{3600}}
Pediatric Dosage Calculation Methods
1. Clark’s Rule
Child Dose=Weight (lb)150×Adult Dose\text{Child Dose} = \frac{\text{Weight (lb)}}{150} \times \text{Adult Dose}
2. Young’s Rule
Child Dose=AgeAge+12×Adult Dose\text{Child Dose} = \frac{\text{Age}}{\text{Age}+12} \times \text{Adult Dose}
Common Dosage Calculation Examples
Example 1
Order: 500 mg
Available: 250 mg
Answer: 2 tablets
Example 2
Order: 100 mg
Available: 50 mg per 5 mL
Answer: 10 mL
Example 3
Order: 20 mg/kg
Weight: 15 kg
Answer: 300 mg
Common Mistakes in Dosage Calculation
Dosage calculation is a critical skill in healthcare, and even small errors can lead to serious consequences. Many students and healthcare professionals make mistakes not because they lack knowledge, but due to carelessness, confusion, or improper understanding of basic concepts. Recognizing these common mistakes in dosage calculation also in pharma calculation is the first step toward avoiding them and ensuring safe medication administration.
Below are the most common dosage calculation mistakes explained in detail:
1. Wrong Unit Conversion
Incorrect unit conversion is one of the most frequent and dangerous errors in dosage calculation.
Why it happens:
- Confusion between units like mg, g, mcg
- Not converting liters to milliliters
- Mixing up hours and minutes
Examples:
- 1 g = 1000 mg
- 1 mg = 1000 mcg
- 1 L = 1000 mL
Common Error:
A doctor prescribes 500 mg, but the student calculates using grams without converting:
500 mg = 0.5 g (if not converted, result will be wrong)
Impact:
This can lead to a 10x or 100x dosing error, which is extremely dangerous.
Best Practice:
- Always convert units before starting calculation
- Write units clearly at each step
- Double-check conversions before final answer
2. Incorrect Formula Usage
Using the wrong formula is another major cause of dosage calculation mistakes.
Why it happens:
- Lack of clarity about different formulas
- Jumping directly into calculation without planning
Correct Formula:
Dose to be given=Prescribed DoseAvailable Dose×Quantity\text{Dose to be given} = \frac{\text{Prescribed Dose}}{\text{Available Dose}} \times \text{Quantity}
Common Error:
Using IV flow rate formula instead of dosage formula.
Example:
Prescribed dose = 500 mg
Available = 250 mg tablet
Correct:
(500 ÷ 250) × 1 = 2 tablets
Impact:
Wrong formula leads to completely incorrect dosage.
Best Practice:
- Identify what is asked before solving
- Write the formula first
- Then substitute values step-by-step
3. Decimal Errors
Decimal placement errors are small but extremely dangerous in dosage calculation.
Why it happens:
- Carelessness during calculation
- Misreading numbers
Examples:
- 0.5 written as 5
- 1.0 written as 10
Impact:
- 10x overdose or underdose
- Serious harm to patient
Clinical Rule:
- Never skip leading zero (write 0.5, not .5)
- Avoid trailing zero (write 1, not 1.0)
Best Practice:
- Always double-check decimal placement
- Recalculate if result looks unusual
- Compare with expected range
4. Misreading Prescription
Misreading the doctor’s order is a very common and serious mistake.
Why it happens:
- Poor handwriting
- Rushing during reading
- Not paying attention to details
Examples:
- Reading 100 mg as 1000 mg
- Confusing OD (once daily) with BD (twice daily)
Impact:
- Incorrect dose administration
- Potential patient harm
Best Practice:
- Read prescription carefully at least twice
- Clarify unclear instructions
- Cross-check drug name, dose, and frequency
Tips to Master Dosage Calculation Formula
- Practice daily
- Memorize formulas
- Double-check units
- Use step-by-step method
Importance of Dosage Calculation
Dosage calculation is a fundamental skill in pharmacy, nursing, and clinical practice. It ensures that patients receive the correct amount of medication based on their condition, age, weight, and medical requirements. The dosage calculation formula plays a crucial role in translating a doctor’s prescription into an accurate and measurable dose.
In healthcare settings, even a small error in dosage can lead to serious consequences. Therefore, understanding the importance of dosage calculation is essential for safe, effective, and professional patient care.
1. Ensures Patient Safety
Patient safety is the primary reason why accurate dosage calculation is important. Medications act directly on the body, and incorrect doses can cause harm.
Why it matters:
- Overdose can lead to toxicity, organ damage, or life-threatening reactions
- Underdose may result in ineffective treatment and delayed recovery
Example:
A small miscalculation in pediatric dosing can be especially dangerous because children require precise weight-based dosing.
Key Point:
Accurate dosage calculation helps ensure that the patient receives the right drug in the right amount at the right time.
Read more- Best calculation formula must know in pharma
2. Prevents Medication Errors
Medication errors are a major concern in healthcare, and incorrect dosage calculation is one of the leading causes.
Common errors include:
- Wrong dose
- Wrong frequency
- Incorrect unit conversion
Impact:
- Adverse drug reactions
- Treatment failure
- Increased hospital stay
How dosage calculation helps:
By applying the correct dosage calculation formula and verifying results, healthcare professionals can significantly reduce medication errors.
3. Improves Treatment Outcomes
Correct dosage directly affects how well a treatment works. Accurate calculations ensure that the drug reaches its therapeutic level in the body.
Benefits:
- Faster recovery
- Effective disease management
- Reduced complications
Example:
In antibiotics, an accurate dose ensures proper infection control, while incorrect dosing can lead to resistance.
4. Supports Individualized Therapy
Every patient is different, and dosage calculation allows healthcare providers to adjust medication based on individual factors.
Factors considered:
- Body weight
- Age
- Organ function (kidney/liver)
- Severity of disease
Importance:
This personalized approach improves safety and effectiveness of treatment.
5. Builds Professional Confidence
Strong knowledge of dosage calculation increases confidence among healthcare professionals.
Benefits:
- Reduces stress during clinical practice
- Improves decision-making
- Enhances accuracy and efficiency
6. Ensures Legal and Ethical Responsibility
Healthcare professionals are legally responsible for administering the correct dose.
Importance:
- Prevents negligence
- Maintains professional standards
- Builds trust with patients
Advanced Dosage Calculations
Advanced dosage calculations are essential in clinical and hospital settings where medications are administered through intravenous (IV) routes. These calculations require a deeper understanding of formulas, units, and patient-specific factors. Unlike basic dosage calculations, advanced calculations are often used in critical care, emergency medicine, and intensive care units, where accuracy is extremely important.
Two of the most important types of advanced dosage calculations are IV dosage calculation and infusion rate calculation.
1. IV Dosage Calculation
IV dosage calculation is used when medications or fluids are administered directly into the bloodstream through intravenous therapy. This method provides rapid drug action, making it essential in emergency and critical care situations.
Why it is important:
- Provides immediate therapeutic effect
- Allows precise control of drug levels
- Commonly used in hospitals and ICUs
Basic IV Dosage Formula
IV Dose Rate=Total DoseTime\text{IV Dose Rate} = \frac{\text{Total Dose}}{\text{Time}}
Example:
A patient needs 1000 mL IV fluid over 10 hours.
Solution:
1000 ÷ 10 = 100 mL/hr
Key Considerations:
- Check units (mL, hours)
- Ensure correct drug concentration
- Monitor patient response
Clinical Importance:
IV dosage calculation is critical because incorrect rates can lead to fluid overload or insufficient drug delivery.
2. Infusion Rate Calculation
Infusion rate calculation determines how fast a drug or fluid should be administered through an IV line. It is especially important in critical care where medications must be delivered at a controlled rate.
Infusion Rate Formula (mL/hr)
Infusion Rate=Volume (mL)Time (hours)\text{Infusion Rate} = \frac{\text{Volume (mL)}}{\text{Time (hours)}}
Drop Rate Formula (gtt/min)
Drop Rate=Volume (mL)×Drop FactorTime (minutes)\text{Drop Rate} = \frac{\text{Volume (mL)} \times \text{Drop Factor}}{\text{Time (minutes)}}
Example:
500 mL IV fluid over 5 hours, drop factor = 20 gtt/mL
Solution:
- Convert time: 5 hours = 300 minutes
- Apply formula:
(500 × 20) ÷ 300 = 33.3 ≈ 33 gtt/min
Why it is Important:
- Ensures correct drug delivery rate
- Prevents overdose or underdose
- Maintains fluid balance
3. Weight-Based Infusion Calculation
Some drugs are administered based on body weight.
Formula:
Dose Rate=Weight (kg)×Dose per kg\text{Dose Rate} = \text{Weight (kg)} \times \text{Dose per kg}
Example:
Drug order: 5 mg/kg/hr
Patient weight: 60 kg
Solution:
60 × 5 = 300 mg/hr
4. Continuous Infusion Calculation
Used for drugs like insulin, heparin, and vasopressors.
Key Points:
- Requires constant monitoring
- Dose adjusted based on patient response
- Common in ICU settings
Common Challenges in Advanced Calculations
- Unit conversion errors
- Incorrect drop factor
- Misinterpretation of prescription
- Calculation under pressure
Tips for Accurate Advanced Dosage Calculations
- Always double-check units
- Write formulas before solving
- Convert time correctly
- Use calculators for accuracy
- Monitor patient response
Conclusion
Dosage calculation formula is an essential skill in healthcare that directly impacts patient safety and treatment effectiveness. Accurate calculations ensure that patients receive the correct amount of medication based on their individual needs, helping to prevent serious complications such as overdose or underdose. For both students and healthcare professionals, mastering dosage calculation is not just an academic requirement but a critical responsibility in clinical practice.
By understanding key pharma calculation topics formulas and applying them correctly, it becomes easier to convert prescriptions into accurate doses. Regular practice plays a major role in building confidence and improving speed, especially in high-pressure clinical environments where quick and precise decisions are required. Developing a habit of solving problems step-by-step and double-checking results further reduces the chances of errors.
In addition, attention to detail—such as proper unit conversion, correct formula selection, and careful reading of prescriptions—is crucial for maintaining accuracy. These small but important steps help ensure that calculations are reliable and consistent in real-life situations.
As healthcare continues to advance, the importance of accurate dosage calculation remains constant. Professionals who are skilled in dosage calculations are better equipped to provide safe, effective, and high-quality patient care. Continuous learning, practice, and adherence to standard calculation methods will help maintain excellence in medication administration and support better clinical outcomes.
FAQs
1. What is dosage calculation formula?
It is a formula used to calculate correct medication dose.
2. Why is dosage calculation important?
To ensure patient safety and correct treatment.
3. What is the basic formula?
Dose = Prescribed ÷ Available × Quantity
4. What is weight-based dosing?
Dose calculated based on body weight.
5. How to avoid mistakes?
Practice and double-check units.